
Hysteroscopic Polypectomy in India for International Patients
Hysteroscopic Polypectomy in India is a scarless fix for polyps. GetWellGo manages your visa and stay for a quick, safe recovery. Stop abnormal bleeding.
Read MoreBest hospitals for Vaginal Brachytherapy treatment & recovery. Trusted care with GetWellGo for international patients seeking advanced treatment.

Category
GynecologyPublished By
GetWellGo TeamUpdated on
20-May-2025Vaginal brachytherapy is an internal radiation therapy that is most commonly applied for the treatment of gynecologic malignancies, notably endometrial (cancer of the uterus) and, in certain instances, vaginal or cervical cancer. It's a highly localized and target-specific treatment aimed to destroy cancerous cells while exposing healthy tissues to minimal irradiation.
Brachytherapy using the vagina is normally well-tolerated, but as with any type of radiation therapy, side effects result from it, which differ according to the amount of radiation, frequency, and personal sensitivity.
These are mostly localized and temporary:
Vaginal Side Effects
Bowel and Bladder Side Effects
What is vaginal brachytherapy?
Vaginal brachytherapy places a source of radiation within or close to the vagina, usually in the form of a cylindrical applicator. It enables a high dose of radiation to be delivered locally to the target site, for example, the vaginal cuff (upper end of the vagina, usually after a hysterectomy), with fewer side effects than external beam radiation therapy.
Vaginal brachytherapy is a typical treatment given either after an operation for endometrial (uterine) cancer or vaginal/cervical cancer.
Initial Consultation
Treatment Planning (using simulation and CT images)
Treatment Sessions
All sessions contain the following parts:
Applicator Insertion
Radiation Delivery
Post-Treatment
Treatment Schedule
Typical regimens:
Following the surgery, brachytherapy is commonly used for endometrial cancer to lower the risk of cancer returning in the upper vagina for early to intermediate stages of the disease.
What is it?
Used after a total hysterectomy for reasons such as:
In some cases, the term may be substituted with another name:
Most women who get vaginal brachytherapy are able to handle it well and are permitted to go home right after the procedure. It usually takes little time to recover, as this treatment is usually given alone (with no added radiation).
During treatment: The time for a session is 30-60 minutes. Most activities can be resumed that very day.
First 1 to 2 days: There may be minor discomfort inside the vagina, some light bleeding or tiredness. The majority of people feel okay after a day.
1week Post-treatment: You should feel fully energized and most irritation in your bladder or bowel should be gone.
2-4 weeks Post-treatment: You could be told to use vaginal dilators to prevent narrowing.
Long-term: Sexual intercourse may be continued after about 4–6 weeks (though your doctor may advise starting earlier). Mild dryness of the vagina may not go away but is easy to handle.
The price of vaginal brachytherapy in India depends on various important factors. Here are some details on what affects the overall price:
Appropriate use of vaginal brachytherapy after surgery for cancer of the uterus gives a high chance of recovery.
One of the features of Artemis Hospital in Gurgaon is that it offers advanced cancer treatment, with vaginal brachytherapy. At the Artemis Cancer Centre, many oncology services are offered, mixed with modern technology and a team of different experts. Important features here include advanced HDR brachytherapy, a team of skilled oncologists and whole-person care. Artemis carries the JCI and NABH accreditation.
In Gurugram’s Medanta Hospital, patients can receive vaginal brachytherapy which uses the HDR brachytherapy method and the MAOLO template (Medanta Anterior Oblique Lateral Oblique) is a new device created to boost the success of brachytherapy for advanced cervical cancers. With Dr. Tejinder Kataria and Dr. Susovan Banerjee leading the way, Radiation Oncology experts at the hospital apply technology and specific treatments for the best hope of success.
The Fortis Memorial Research Institute (FMRI) in Gurgaon is regarded as a top hospital for its top-quality oncology care such as vaginal brachytherapy. In the Radiation Oncology department, High-Dose Rate (HDR) brachytherapy is used for accurate treatment of cervical and endometrial cancers. Because of its multidisciplinary approach, FMRI can ensure that personalized care plans are given to all patients.
Max Super Speciality Hospital in Saket, New Delhi, treats cancer patients with its Max Institute of Cancer Care (MICC). The treatment delivers radiation in a high dose that is precise to the tumor but protects healthy tissues. At the hospital, teams of doctors in different fields work together, allowing personal care for every patient. Being nationally accredited by several bodies, including the National Accreditation Board for Hospitals & Healthcare Providers and the National Accreditation Board for Testing and Calibration Laboratories, Max Super Speciality Hospital focuses on patients’ needs.
At Indraprastha Apollo Hospital in Delhi, doctors use vaginal brachytherapy for the treatment of cancers in the uterus and cervix. The establishment relies on HDR brachytherapy for patients, makes sure to unite surgical, medical and radiation oncology care and regularly supports and educates the patients going through the procedure.
Many gynecologic cancers such as those of the uterus, cervix, vagina, vulva and ovaries, can be treated with radiation therapy. This treatment uses X-rays or protons to eliminate cancer cells or hinder their growth.
External Beam Radiation Therapy (EBRT)
Brachytherapy
Stereotactic Body Radiation Therapy (SBRT)
Intraoperative Radiation Therapy (IORT)

Hysteroscopic Polypectomy in India is a scarless fix for polyps. GetWellGo manages your visa and stay for a quick, safe recovery. Stop abnormal bleeding.
Read More
Laparoscopic Myomectomy in India saves your uterus. We safely remove fibroids to protect your fertility. GetWellGo handles your medical visa and stay.
Read More
Sickle Cell Anemia and Pregnancy in India for Nigerian Patients is managed safely. GetWellGo ensures expert care for a healthy delivery. Start your journey.
Read More.png)
Choose GetWellGo for advanced umbilical artery catheterization. World-class newborn care trusted by international families for safety, comfort, and results.
Read More
Vaginal dilatation care in India helps global patients restore health and confidence. Expert gynecologists, modern techniques, and affordable care ensure safe and effective treatment.
Read More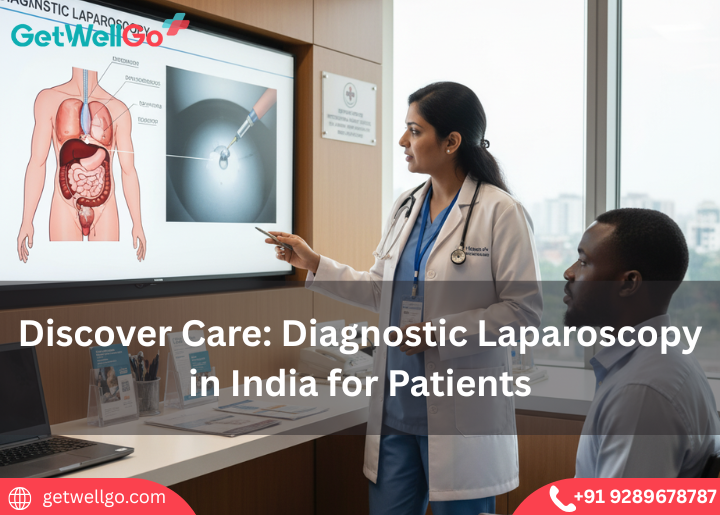
Discover Care with GetWellGo: Affordable diagnostic laparoscopy in India for international patients. Expert care, advanced tech & seamless support.
Read More
GetWellGo helps international patients access top pelvic organ prolapse treatment in India with expert care, advanced surgery & complete support.
Read More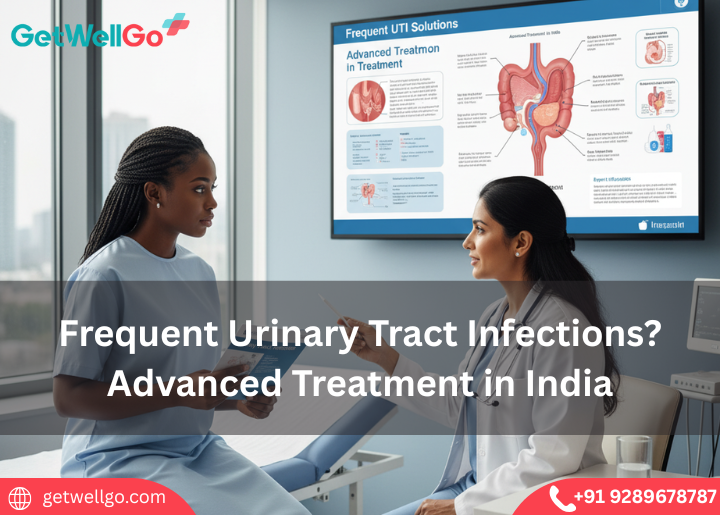
Struggling with recurrent UTIs? GetWellGo helps international patients access advanced urinary tract infection treatments in India with trusted specialists.
Read More

World-class PCOS treatment in India with GetWellGo. Affordable care, advanced medical expertise, and full support for international patients.
Read More
Dreaming of a family? Explore safe, affordable Intrauterine Insemination (IUI) treatment in India with GetWellGo, trusted by international patients.
Read More
Myomectomy surgery in India provides advanced, safe, and affordable solutions for fibroid removal. Top hospitals ensure expert care, modern techniques, and faster recovery for women’s health.
Read MoreFill the form below to get in touch with our experts.
Please fill in your details below and our experts will get back to you.