
Hysteroscopic Polypectomy in India for International Patients
Hysteroscopic Polypectomy in India is a scarless fix for polyps. GetWellGo manages your visa and stay for a quick, safe recovery. Stop abnormal bleeding.
Read MoreSickle Cell Anemia and Pregnancy in India for Nigerian Patients is managed safely. GetWellGo ensures expert care for a healthy delivery. Start your journey.

Category
GynecologyPublished By
GetWellGo TeamUpdated on
29-Jan-2026Sickle cell anemia is a hereditary disease that causes volume depletion in red blood cells. Typically round and flexible, red blood cells become rigid, forming a crescent or sickle shape in SCA. These abnormally shaped cells can block blood flow, which causes pain, organ damage, and a greater vulnerability to infections. Pregnancy and sickle cell anemia is high-risk as both mother and fetus have higher chances to suffer complications. But close medical supervision and care, pregnancy in women with SCA is feasible and most of them are able to have successful pregnancies.
Sickle Cell Anemia and Pregnancy are interrelated because pregnancy puts more strain on the body and can worsen SCA problems. Conversely, pregnancy is impacted by Sickle cell anemia by the things it has an effect on such as blood flow, oxygen levels and organ functions.
This synchronization means:
Sickle cells are sticky, and tend to clog blood vessels
Can reduce placental blood flow during pregnancy causing:
SCA is inherited. An expectant mother with SCA can pass the gene to her child.
If both parents have the sickle cell trait, there's a:
The following is an in-depth plan on sickle cell anemia and pregnancy that is applicable to the needs of Nigerian patients seeking care in India:
Pregnant women who are affected with sickle cell anemia (SCA) have a high risk of having medical problems since:
The general best practices in the management of sickle cell in pregnancy are usually:
India is a country where patients in Nigeria and other nations usually seek elaborate medical treatment due to:
Nigerian patients seeking treatment in India require a visa of the type of Visa Medical Visa which they should usually back up with:
High-risk pregnancy is observed in women with sickle cell anemia (HbSS), as well as other severe forms of SCD. Tertiary care centers in India provide combined services of hematology and maternal-fetal medicine where Nigerian patients, which usually harbour more severe genotypes, are given.
Delivery-Related Complications
The cost of managing a sickle cell crisis during pregnancy can take widely different amounts of money depending on the complexity of medical care, type of hospital used and duration of treatment. As such cases are categorized as the high-risk obstetric emergencies; costs are usually higher than the normal antenatal packages.
Basic transfusion involves laboratory, blood unit and monitoring expenses.
Exchange transfusions (applied in case of severe complications are more costly because of:
Repeated:
The high-risk pregnancies demand more frequent testing which adds to overall bills.
Preterm birth or fetal distress may necessitate:
These additional expenses are common to the Nigerian patient:
Normal delivery is less expensive through vaginal means.
Emergency or scheduled cesarean section incurs additional costs because of:
Pregnancy is a predisposing factor for increased blood volume and iron demand. This natural change worsens chronic hemolytic anemia in those with sickle cell disease (SCD), especially HbSS (sickle cell anemia), and these pregnancies are high risk and require specialist care.
Key Mechanisms:
Pregnant women with sickle cell anaemia (HbSS) or other severe phenotypes of the disease also have markedly increased risks of maternal and fetal complications. Usually these cases are managed with multidisciplinary care using protocols in tertiary hospitals in India.
Most developed Indian hospitals offer coordinated care by:
Monitoring Regularly
Preventive Measures
Pain & Crisis Management
Blood Transfusion Strategy
Symptomatic anemia or fetal compromise Simple transfusion.
Transfuse with extreme complications including:
There are centers that employ prophylactic transfusion on women who experience recurrent crises or have poor obstetric history.
Partner testing (among these are Hb electrophoresis or genetic testing)
In case both parents are carriers of sickle genes:
Newborn screening and early pediatric follow-up counselling.
Close monitoring for:
Neonatal:
These are the results of pregnancy of women with sickle cell disease (SCD) in India - with an Indian context regarding African (e.g., Nigerian) patients wanting treatment or counselling:
These results demonstrate considerably high risks, which suggests the absent perfection (e.g. >90% uncomplicated) of the success rates is typical in nature/untreated environments.
Pregnancy with sickle cell disease is a high-risk clinical situation for maternal complications, such as anemia, vaso-occlusive crisis, acute chest syndrome, infections, and hypertensive disorders, and fetal complications including preterm birth, growth retardation, and stillbirth. Tertiary hospitals with multidisciplinary teams, well-equipped blood transfusion services, intensive care, maternal and neonatal care, genetic counselling and an established system of antenatal monitoring can be a beacon of hope for African and specifically Nigerian patients who come to India for treatment, immensely improving their chances of survival and successful delivery. Although standardized success rates are not consistently reported, there is always evidence to support the idea that the most important determinants of attaining positive maternal and neonatal outcomes among this risk group of the population are early referral, ongoing specialist care, timely post-partum management of complications, and a planned delivery in a properly equipped center.
GetWellGo is regarded as a leading supplier of healthcare services. We help Nigerian patients choose the best treatment locations that suit their needs both financially and medically.
We offer:

Hysteroscopic Polypectomy in India is a scarless fix for polyps. GetWellGo manages your visa and stay for a quick, safe recovery. Stop abnormal bleeding.
Read More
Laparoscopic Myomectomy in India saves your uterus. We safely remove fibroids to protect your fertility. GetWellGo handles your medical visa and stay.
Read More.png)
Choose GetWellGo for advanced umbilical artery catheterization. World-class newborn care trusted by international families for safety, comfort, and results.
Read More
Vaginal dilatation care in India helps global patients restore health and confidence. Expert gynecologists, modern techniques, and affordable care ensure safe and effective treatment.
Read More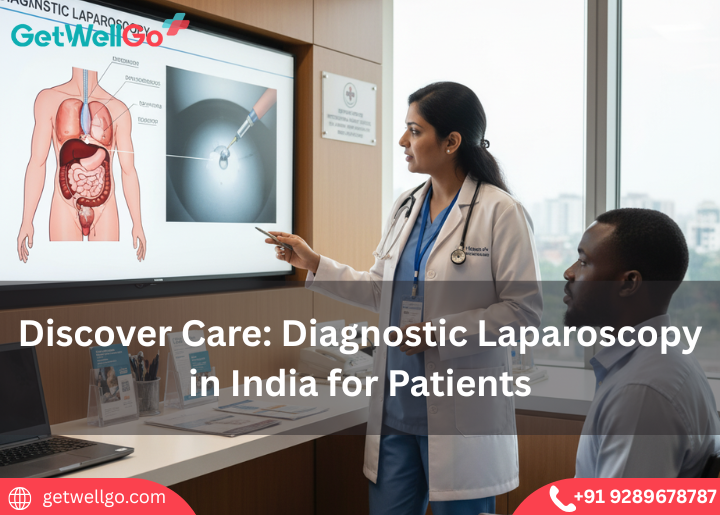
Discover Care with GetWellGo: Affordable diagnostic laparoscopy in India for international patients. Expert care, advanced tech & seamless support.
Read More
GetWellGo helps international patients access top pelvic organ prolapse treatment in India with expert care, advanced surgery & complete support.
Read More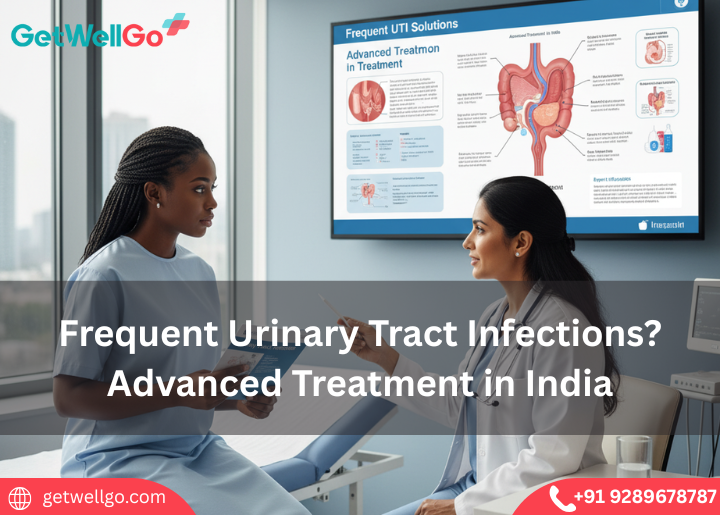
Struggling with recurrent UTIs? GetWellGo helps international patients access advanced urinary tract infection treatments in India with trusted specialists.
Read More

World-class PCOS treatment in India with GetWellGo. Affordable care, advanced medical expertise, and full support for international patients.
Read More
Dreaming of a family? Explore safe, affordable Intrauterine Insemination (IUI) treatment in India with GetWellGo, trusted by international patients.
Read More
Myomectomy surgery in India provides advanced, safe, and affordable solutions for fibroid removal. Top hospitals ensure expert care, modern techniques, and faster recovery for women’s health.
Read More.png)
GetWellGo connects international patients with India’s top hospitals for laparoscopic hysterectomy. Expert care & advanced surgery at affordable costs.
Read MoreFill the form below to get in touch with our experts.
Please fill in your details below and our experts will get back to you.